
Pain radiating from the hip to the leg can be debilitating, significantly impacting daily activities. This pain can be a symptom of various health conditions ranging from minor injuries to chronic illnesses. The complexity of the musculoskeletal system, with its interconnected network of bones, muscles, tendons, and nerves, provides multiple potential sources of pain. Understanding these potential causes can guide the patient and healthcare professional towards a more accurate diagnosis and effective treatment.
Hip Anatomy and How it Relates to Leg Pain

- The hip is one of the body’s largest weight-bearing joints, made up of the hip socket and the femoral head.
- The hip socket is part of the pelvic bone, while the femoral head is the top part of the thigh bone or femur.
- These bones are cushioned by a layer of articular cartilage, allowing for smooth movement.
- The hip joint is encased in a capsule lined with a thin membrane called the synovium, which produces lubricating synovial fluid.
- The joint is surrounded by various soft tissues, including muscles, tendons, and ligaments, which provide strength and stability.
- Any disruption to these structures, due to injury, overuse, or disease, can cause hip pain.
- Hip pain that radiates to the leg is often due to irritation of nearby nerves caused by inflammation or injury to the muscles or tendons.
- The proximity of the hip joint to the sciatic nerve, which serves the legs, makes the hip susceptible to conditions causing radiating pain.
The Nerves Involved in Transmitting Pain from Hip to Leg
Several nerves are involved in transmitting pain from the hip down to the leg. These include:
Sciatic Nerve: This is the largest nerve in the body, originating from the lumbar spine’s lower segments and running through the buttocks and down the back of the leg It is responsible for motor and sensory functions in the leg (5). It provides sensation to the skin and controls the muscles of the lower leg and feet. Conditions such as sciatica (where the sciatic nerve is compressed or irritated) can cause pain radiating from the hip down the leg.
Femoral Nerve: This nerve arises from the lower part of the lumbar spine and runs down the front of the thigh. It controls the muscles that help straighten the leg and those that assist in hip bending. Damage or compression to the femoral nerve can also result in pain radiating down the front of the leg.
Obturator Nerve: Originating from the lumbar region, this nerve passes through the pelvic region and down the inner thigh. It helps control the adductor muscles that pull the legs together. Conditions affecting the obturator nerve can lead to pain in the hip and inner thigh.
Superior and Inferior Gluteal Nerves: These nerves, arising from the sacral spine, supply the gluteal muscles in the buttocks. They can become irritated or compressed due to various conditions, including trauma, leading to hip and possibly radiating leg pain (4).
Pudendal Nerve: Although it’s primarily associated with pelvic functions, irritation or compression of the pudendal nerve (which also arises from the sacral spine) can sometimes cause pain that is referred to the hip region.
Each of these nerves can be affected by various conditions, such as disc herniation, spinal stenosis, nerve entrapment syndromes, or nerve inflammation. Therefore, a comprehensive understanding of the anatomy and function of these nerves is crucial in diagnosing and treating hip to leg pain.
Read More: The best treatment of PLID/ Disc herniation / Disc prolapse in Bangladesh
Referred Pain from Hip to Leg
Referred pain is a phenomenon in which pain is perceived at a location different from the site of the painful stimulus. This occurs because of the complex network of sensory nerves that relay pain signals to the brain. If the pathway of a nerve is irritated or compressed at one point, the brain may interpret that the pain is coming from a different location along that pathway.
In the context of hip to leg pain, referred pain can occur when a problem in the hip joint or nearby structures produces pain that is felt down the leg (6). For instance, hip arthritis or a hip labral tear can cause pain that radiates to the groin, thigh, or knee. Understanding the concept of referred pain is crucial because it can sometimes mislead the diagnostic process. A thorough examination and history-taking are therefore vital in distinguishing referred pain from pain originating in the leg itself.
Causes of Hip Pain Radiating Down the Leg
A. Sciatica
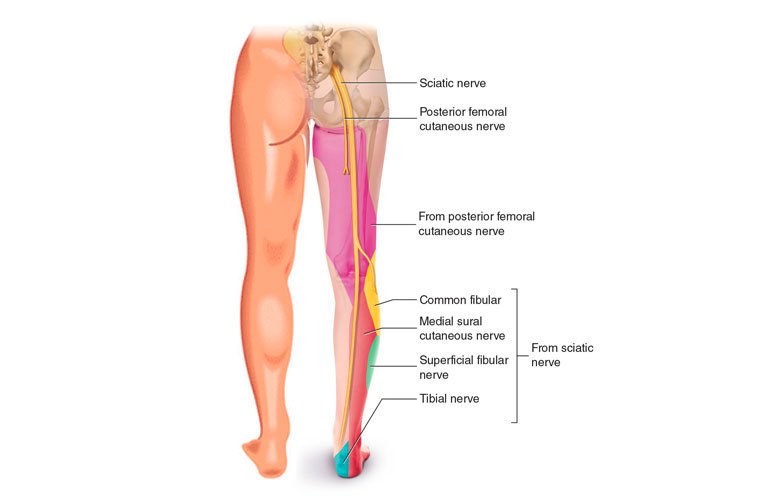
Definition and Explanation of Sciatica
Sciatica is a phrase used to describe pain, numbness, and weakness that go down each leg along the sciatic nerve from the lower back through the hips and buttocks. Herniated discs, bone spurs on the spine, and spinal stenosis are common causes that typically only affect one side of the body. Spinal stenosis compresses a portion of the nerve while causing irritation to the lower lumbar and lumbosacral spine’s nerve root (7).
Symptoms and How it Results in Hip to Leg Pain
- Pain that travels from the lower (lumbar) spine to the buttock and down the back of the leg is the main sign of sciatica.
- The discomfort can range from a subtle ache to a searing, burning sensation, and it can be mild or severe. It can occasionally feel like an electric shock or jolt. Frequently, extended sitting, coughing, or sneezing make the pain worse.
- Numbness, tingling, or muscle weakness in the affected leg or foot are additional typical symptoms.
- It is possible to feel numbness in one area of the leg while experiencing pain in another.
- Sciatica pain may begin suddenly or gradually.
- Some people experience pain constantly, while others only occasionally, therefore the degree and frequency of the pain might vary.
Common Causes of Sciatica such as Disk Herniation and Spinal Stenosis
Disk Herniation: This condition is one of the most common causes of sciatica. The discs in the spine are rubbery cushions between the individual bones (vertebrae). A disc may develop a small crack or tear and bulge into the spinal canal, a situation known as a herniated or slipped disc. This herniation can irritate the nearby nerve root, leading to sciatica.
Spinal Stenosis: This condition occurs when the spinal canal narrows with age. This narrowing can compress and irritate the nerves that exit the spinal cord, including the sciatic nerve. This compression can result in symptoms of sciatica.
Other causes can include spinal tumors, infections, abscesses, or other conditions like piriformis syndrome, where the piriformis muscle (a small muscle located deep in the buttock) irritates the sciatic nerve. However, disc herniation and spinal stenosis are the most common causes.
The pain from these conditions often originates in the hip and radiates down the leg due to the path of the sciatic nerve. They can lead to inflammation, pain, and often some numbness in the affected limb.
B. Hip Disorders
1. Osteoarthritis of the Hip

Osteoarthritis (OA) of the hip is a chronic condition characterized by the breakdown of the cartilage that cushions the ends of the bones where they meet to form joints. In the hip, this loss of cartilage can cause the bones of the joint to rub together, resulting in pain, stiffness, and loss of joint movement. This condition often affects individuals over the age of 50 but can occur in younger people as well.
Pain from hip osteoarthritis typically feels like a “deep” ache localized in the groin, thigh, buttock, and sometimes, the knee. It can radiate down the thigh and cause difficulty walking and moving about.
2. Labral Tear in the Hip
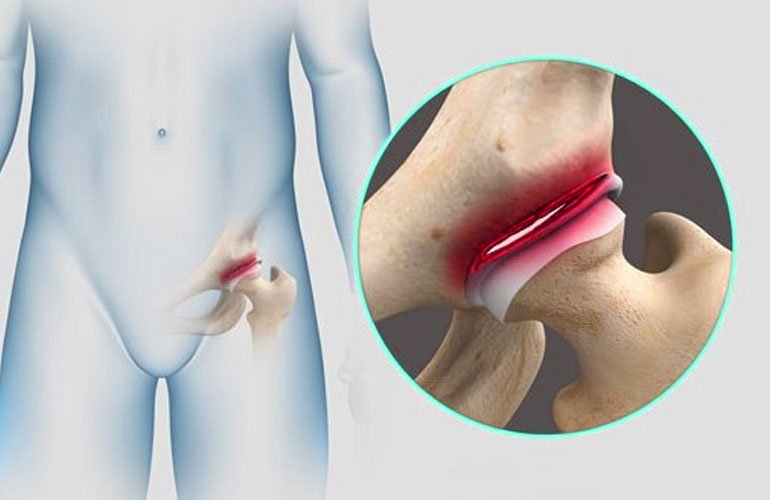
The labrum is a ring of cartilage that follows the outside rim of the hip joint socket. Its purpose is to provide stability to the joint by deepening the socket and to aid in shock absorption. A tear in the labrum, often due to trauma, repetitive movements, or degenerative changes, can cause pain and discomfort.
A hip labral tear may cause pain in the groin area or the outer hip. Some people feel a locking, clicking, or catching sensation in the hip joint when they move it. This pain can radiate down the leg as well (3).
3. Iliopsoas bursitis
Bursitis is the inflammation of small fluid-filled sacs, called bursae, that act as cushions between bones and soft tissues. The iliopsoas muscle, a hip flexor located in the front part of the hip, has an associated bursa that can become inflamed, often due to overuse.
Iliopsoas bursitis can cause pain in the hip area, particularly with activities such as walking or climbing stairs. This pain can radiate down towards the thigh.
4. Hip Snapping syndrome
This condition, also known as external snapping hip syndrome, occurs when a tendon or muscle slides over a bony protrusion in your hip. It’s often harmless and painless. But in some people, it can lead to hip pain, especially with certain movements.
The most common symptom of snapping hip syndrome is a snapping sensation or popping noise in the hip when walking, getting up from a chair, or swinging the leg around. This can be accompanied by pain and discomfort, sometimes radiating down the leg.
Read More: 6 Tips for Relieving Pain From Herniated Discs or Disc Prolapse
5. Hip Bursitis
In general, hip bursitis refers to inflammation of any of the bursae in the hip area. The most common type is trochanteric bursitis, affecting the bursa located on the outside (lateral area) of your hip. This can be due to overuse, injury, or an underlying condition like arthritis or a hip injury.
Trochanteric bursitis typically causes pain on the outside of your hip, which can extend down the side of the leg to the knee. This pain can be sharp and intense during initial onset, then may turn into a dull and achy sensation later. Activities such as climbing stairs, running, or even lying on the affected side can exacerbate the pain.
C. Miscellaneous Causes
1. Sacroiliitis

Sacroiliitis is inflammation of one or both of your sacroiliac joints — the places where your lower spine and pelvis connect. This condition can cause pain in your buttocks or lower back, and may even extend down one or both legs, often mimicking sciatic pain. It can be caused by various forms of arthritis, trauma, or infection.
2. Piriformis Syndrome

The piriformis muscle, which is located in the area of the buttocks, spasms and causes buttock pain in Piriformis syndrome, a neuromuscular disorder. Similar to sciatica, the piriformis muscle can irritate the neighboring sciatic nerve, causing pain, numbness, and tingling to radiate down the back of the leg and into the foot. (2).
3. Spinal Tumors

Spinal tumors are abnormal growths of tissue found in and around the spine. They can be benign (noncancerous) or malignant (cancerous). When these tumors impinge on nerves, including the sciatic nerve, they can cause pain that radiates from the hip down the leg. While they are relatively rare, they represent a serious condition that requires immediate medical attention (1).
4. Injuries or Infections
Hip pain that radiates to the leg can also be caused by injuries such as sprains, strains, fractures, or dislocations. Infections in the hip joint or the tissues around the hip can cause similar pain. Pain caused by these conditions is typically localized to the hip and thigh area but can radiate down the leg in certain instances (8).
5. Wallet Sciatica
Interestingly, lifestyle or habitual factors can contribute to hip and leg pain. One common example is the habit of carrying a large wallet in the back pocket. Sitting on a large wallet for prolonged periods can compress the sciatic nerve (a condition often dubbed “wallet sciatica” or “fat wallet syndrome”) and lead to pain that radiates from the hip down the leg. To prevent this, consider carrying your wallet in a front pocket or a bag instead.
Diagnosing Hip to Leg Pain
Differential Diagnosis:
Other Conditions That Can Cause Similar Symptoms
A. Lumbar spine conditions
Conditions like a herniated disc, lumbar spinal stenosis, or spondylolisthesis can cause compression of the nerves, leading to pain radiating from the hip down the leg, which may mimic hip-originated pain (15).
B. Peripheral vascular disease (PVD)
Characterized by the buildup of fatty deposits in the arteries, PVD can reduce blood flow to the legs and feet, causing pain in the leg or hip when walking, which often resolves with rest (13).
C. Certain neurological conditions
Conditions such as peripheral neuropathy (often associated with diabetes) can cause burning or tingling pain from the hip to the leg, which may be incorrectly attributed to the hip (18). Similarly, conditions like restless leg syndrome or complex regional pain syndrome can present with leg discomfort that may initially be misinterpreted as stemming from the hip.
Importance of Professional Consultation
Given the many potential causes of hip to leg pain, professional consultation is crucial for accurate diagnosis and effective treatment. Primary care providers, orthopedic surgeons, neurologists, and physical therapists are among the healthcare professionals who may be involved in assessing and managing this type of pain.
A healthcare professional will take a detailed history, including the nature, onset, duration, and location of the pain, as well as any related symptoms. They will also consider factors such as the patient’s age, overall health status, lifestyle, and occupational demands.
Procedures in Diagnosing Such as Physical Exams and Imaging Tests
Patient History and Physical Examination
The diagnosis process for hip to leg pain commences with two essential steps:
- Collecting Patient’s Medical History: Detailed information about the onset of pain, the nature of the pain, previous injuries or surgeries, lifestyle habits, and family history of similar issues is gathered.
- Physical Examination: A physical exam will typically involve observing the patient’s posture, gait, and physical movements to identify any abnormalities (16).
Posture: Abnormal posture could indicate underlying musculoskeletal or neurological disorders.
- Hunched or stooped posture, which could indicate conditions like osteoporosis or Parkinson’s disease.
- Asymmetrical posture, which may signal scoliosis or other musculoskeletal issues.
- Unusually rigid or fixed posture, which might be a sign of conditions like ankylosing spondylitis.
Gait: The manner of walking can reveal specific health conditions.
- An antalgic gait, where the patient tries to minimize weight bearing on one side due to pain, might suggest a hip or knee problem.
- A waddling or Trendelenburg gait may point towards hip dysplasia or muscular dystrophy.
Range of Motion: Limitations in joint mobility could signal issues like arthritis or injury.
The Role of Palpation and Provocative Maneuvers
During the physical examination, the doctor may also use palpation (touching or pressing the area) to identify tender areas and provocative maneuvers (specific movements) to provoke symptoms and understand the source of pain better (10).
Imaging Tests: X-rays, MRI, and CT scans

If an underlying condition is suspected, several imaging tests might be ordered:
- X-rays: These are used to identify bone-related problems, like fractures or signs of arthritis.
- MRI and CT scans: These provide more comprehensive images, capturing soft tissues such as muscles, tendons, and nerves. In some cases, computed tomography (CT) scans may also be used (17). They can detect problems like herniated discs, tumors, or structural irregularities.
- Ultrasound: This imaging technique can provide real-time images of the hip joint and surrounding soft tissues. It can be especially useful in diagnosing soft tissue injuries such as bursitis or tendinitis.
Additional Diagnostic Procedures: Nerve Studies and Blood Tests
In certain situations, further diagnostic procedures might be necessary:
- Nerve Studies: Nerve conduction studies or electromyography (EMG) may be used to assess nerve function. They can help diagnose conditions like nerve compression syndromes or peripheral neuropathy.
- Blood Tests: These can identify signs of infection or inflammation, potentially pointing towards conditions like autoimmune diseases, infections, or specific types of cancer (11).
Read More: Top 3 Symptoms Suggesting a Slipped or Bulging Disc or Herniated Disc
Management and Treatment Options for Hip to Leg Pain
Non-Pharmacological Interventions
Non-pharmacological interventions form the cornerstone of managing hip to leg pain, particularly in the initial stages or for mild to moderate conditions. These may include:
Physical Therapy: Physical therapy can help to strengthen the muscles around the hip and improve flexibility and range of motion. It can also help with pain management and reducing the risk of future injuries (12)
- Strengthening Exercises: PT often includes exercises to strengthen the muscles around the hip joint. Strengthening these muscles can provide better support for the hip joint and relieve stress on it, thereby reducing pain. For instance, if the cause of hip to leg pain is arthritis, exercises focusing on strengthening the quadriceps, hamstrings, and gluteal muscles can help.
- Flexibility Exercises: Increasing the flexibility of your hip and leg muscles can help reduce stiffness and increase your range of motion. This could involve stretches for your hip flexors, hamstrings, and piriformis muscle.
- Manual Therapy: Physical therapists may also use hands-on techniques to help reduce pain and increase flexibility. This could include massage, joint mobilizations, and myofascial release.
- Gait and Balance Training: If the hip to leg pain is affecting your ability to walk or maintain balance, a physical therapist can work with you on exercises to improve these skills.
- Modalities: Physical therapists can use various modalities to help reduce pain and inflammation, such as heat and cold therapy, ultrasound, electrical stimulation, and traction.
- Patient Education: Education about the condition and how to manage it is a vital part of physical therapy. This may involve teaching you about proper body mechanics during daily activities to prevent further injury, recommending assistive devices if needed (like a cane or walker), and providing guidance on a home exercise program.
A physical therapy program should be individualized to each patient’s specific needs and capabilities. A physical therapist can provide a thorough evaluation and design a program that targets your specific weaknesses or deficits. Keep in mind that consistent participation and adherence to the recommended exercises and lifestyle changes are key for the best outcomes in physical therapy.
Lifestyle Modifications: This may include weight loss (for overweight or obese patients), ergonomic adjustments (e.g., using a supportive chair), and modifying physical activities that exacerbate the pain.
Application of Heat or Cold: Heat can help relax tense muscles and increase blood flow, while cold can help reduce inflammation and numb pain.
Pharmacological Treatment
When non-pharmacological interventions are not enough to manage pain, medications may be considered. These can include:
non-steroidal anti-inflammatory medications (NSAIDs), paracetamol, or topical analgesics are examples of over-the-counter painkillers.
prescription drugs, including more potent NSAIDs, opioids (for really bad, short-term pain), muscle relaxants, or specific antidepressants or anticonvulsants for nerve pain.
In some circumstances, corticosteroid injections may be utilized to treat the affected area’s pain and reduce inflammation.
Surgical Treatments
Surgical treatments are typically reserved for severe cases or when other treatments have been ineffective (4). The choice of surgery depends on the underlying cause of the hip to leg pain:
- Joint Replacement: For severe hip arthritis causing leg pain, total hip arthroplasty (hip replacement) may be considered.
- Spinal Surgery: For conditions like lumbar spinal stenosis or herniated discs causing sciatic pain, surgeries such as laminectomy or discectomy may be performed.
- Vascular Surgery: In cases of peripheral vascular disease-causing leg pain, procedures to improve blood flow may be necessary.
In conclusion, the management and treatment of hip to leg pain should be tailored to the individual patient, based on the underlying cause of the pain, the severity of symptoms, and the patient’s overall health and preferences.
Conclusion
If there’s one takeaway from this discussion, it is that persistent hip to leg pain should not be ignored. It’s a signal from your body that something isn’t right. While some causes of hip to leg pain are more severe than others, any persistent pain is a reason to seek professional help.
Given the multitude of potential causes, it’s critical to consult a healthcare provider who can guide you towards the right diagnosis and treatment. And, remember: while some causes of hip to leg pain can be effectively treated, prevention through a healthy lifestyle is always the best approach. From regular physical activity and a healthy diet to good posture and ergonomic practices, these daily habits can make a significant difference in maintaining joint health and avoiding hip to leg pain
FAQ’s
-
What are the common causes of hip to leg pain?
Hip to leg pain can result from various causes, including but not limited to: arthritis, hip fractures, bursitis, tendinitis, hip labral tears, sciatica, peripheral neuropathy, lumbar herniated discs, and muscular strains or sprains.
-
Can hip to leg pain be a sign of serious illness?
Yes, hip to leg pain can sometimes indicate serious conditions such as hip fractures, severe arthritis, infections, cancers, or vascular diseases. However, it can also be due to less serious causes. It’s essential to consult a healthcare professional if you’re experiencing persistent or severe pain.
-
What is sciatica and how does it cause hip to leg pain?
Sciatica is a condition characterized by pain that radiates along the path of the sciatic nerve, which branches from your lower back through your hips and buttocks and down each leg. This pain can be caused by compression or irritation of the sciatic nerve or its roots in the lower spine.
-
Can arthritis cause hip to leg pain?
Yes, arthritis, especially osteoarthritis and rheumatoid arthritis, can cause hip to leg pain. Arthritis leads to inflammation and degradation of the joint, which can result in pain and stiffness that extends to the leg.
-
How is hip to leg pain diagnosed?
Diagnosis for hip to leg pain typically involves a medical history review, a physical examination, and imaging tests such as X-rays, CT scans, or MRIs. In some cases, nerve conduction studies might be conducted to diagnose nerve-related causes.
-
How can hip to leg pain be treated?
Treatment depends on the underlying cause. It may include pain relievers, physical therapy, weight management, surgery, and lifestyle modifications like exercise and a balanced diet. In cases of sciatica, epidural steroid injections or even surgery may be recommended.
-
Can hip to leg pain be prevented?
While not all causes of hip to leg pain can be prevented, maintaining a healthy weight, staying physically active, practicing good posture, and avoiding prolonged sitting or standing can help reduce the risk. Regular check-ups can also help identify potential problems early.
-
Can hip to leg pain be a result of physical activity?
Yes, excessive or improper physical activity can lead to conditions like muscle strain, tendinitis, and stress fractures, which can cause hip to leg pain. It’s important to use proper form and equipment when exercising, and to allow your body to rest and recover.
-
Is hip to leg pain common in older adults?
Yes, older adults are more susceptible to conditions like arthritis and fractures, which can cause hip to leg pain. However, this doesn’t mean that younger individuals are immune. Any age group can experience hip to leg pain due to various causes.
-
What type of doctor should I see for hip to leg pain?
You can start with your primary care physician, who might refer you to a specialist such as an orthopedic surgeon, rheumatologist, or neurologist depending on the suspected cause of your pain. Physical therapists may also be involved in the treatment process.
References
1. Gerszten, P.C., Mendel, E. and Yamada, Y., 2009. Radiotherapy and radiosurgery for metastatic spine disease: what are the options, indications, and outcomes?. Spine, 34(22S), pp.S78-S92.
https://journals.lww.com/spinejournal/Fulltext/2009/10151/Image_guided_Hypo_fractionated_Stereotactic.00011.aspx
2. Hopayian, K. and Danielyan, A., 2018. Four symptoms define the piriformis syndrome: an updated systematic review of its clinical features. European Journal of Orthopaedic Surgery & Traumatology, 28, pp.155-164. https://link.springer.com/article/10.1007/s00590-017-2031-8
3. McCormick, F., Nwachukwu, B.U. and Provencher, M.T., 2012. Stress fractures in runners. Clinics in sports medicine, 31(2), pp.291-306. https://www.sportsmed.theclinics.com/article/S0278-5919(11)00102-5/abstract
4. Moore, K.L., Dalley, A.F. and Agur, A.M., 2013. Clinically oriented anatomy. Lippincott Williams & Wilkins. https://books.google.com/books?hl=en&lr=&id=-Le5bc5F0sYC&oi=fnd&pg=PP2&dq=7.%09Moore+KL,+Dalley+AF,+Agur+AM.+Clinically+oriented+anatomy.+Lippincott+Williams+%26+Wilkins%3B+2013+Feb+13.&ots=jMBlP1eswI&sig=lxQelV_AMhCz7KfVazoBFDvwSoM
5. Sekiguchi, M., Kikuchi, S. and Myers, R.R., 2004. Experimental spinal stenosis: relationship between degree of cauda equina compression, neuropathology, and pain. Spine, 29(10), pp.1105-1111.
https://journals.lww.com/spinejournal/fulltext/2004/05150/experimental_spinal_stenosis__relationship_between.11.aspx
6. Suri, P., Morgenroth, D.C. and Hunter, D.J., 2012. Epidemiology of osteoarthritis and associated comorbidities. PM&R, 4, pp.S10-S19. https://onlinelibrary.wiley.com/doi/abs/10.1016/j.pmrj.2012.01.007
7. Valat, J.P., Genevay, S., Marty, M., Rozenberg, S. and Koes, B., 2010. Sciatica. Best practice & research Clinical rheumatology, 24(2), pp.241-252. https://www.sciencedirect.com/science/article/pii/S1521694209001417
8. Watson-Jones, R., 1962. Fractures and joint injuries. E. & S. Livingstone. http://117.239.25.194:7000/jspui/bitstream/123456789/1853/7/INDEX.pdf
9. Allen, W.C. and Cope, R., 1995. Coxa saltans: the snapping hip revisited. JAAOS-Journal of the American Academy of Orthopaedic Surgeons, 3(5), pp.303-308. https://journals.lww.com/jaaos/fulltext/1995/09000/coxa_saltans__the_snapping_hip_revisited.6.aspx
10. Byrd, J.W., 2003. Hip arthroscopy: patient assessment and indications. Instructional Course Lectures, 52, pp.711-719.
https://europepmc.org/article/med/12690896
11. Taksande, B., Ansari, S., Jaikishan, A. and Karwasara, V., 2011. The diagnostic sensitivity, specificity and reproducibility of the clinical physical examination signs in patients of diabetes mellitus for making diagnosis of peripheral neuropathy. Journal of Endocrinology and Metabolism, 1(1), pp.21-26. https://www.jofem.org/index.php/jofem/article/view/6
12. French, H.P., Cusack, T., Brennan, A., Caffrey, A., Conroy, R., Cuddy, V., FitzGerald, O.M., Gilsenan, C., Kane, D., O’Connell, P.G. and White, B., 2013. Exercise and manual physiotherapy arthritis research trial (EMPART) for osteoarthritis of the hip: a multicenter randomized controlled trial. Archives of physical medicine and rehabilitation, 94(2), pp.302-314. https://www.sciencedirect.com/science/article/pii/S0003999312010180
13. Kreiner, D.S., Hwang, S.W., Easa, J.E., Resnick, D.K., Baisden, J.L., Bess, S., Cho, C.H., DePalma, M.J., Dougherty II, P., Fernand, R. and Ghiselli, G., 2014. An evidence-based clinical guideline for the diagnosis and treatment of lumbar disc herniation with radiculopathy. The Spine Journal, 14(1), pp.180-191. https://www.sciencedirect.com/science/article/pii/S1529943013014502
14. Moorman III, C.T., Warren, R.F., Hershman, E.B., Crowe, J.F., Potter, H.G., Barnes, R., O’Brien, S.J. and Guettler, J.H., 2003. Traumatic posterior hip subluxation in American football. JBJS, 85(7), pp.1190-1196.
https://journals.lww.com/jbjsjournal/Fulltext/2003/07000/TRAUMATIC_POSTERIOR_HIP_SUBLUXATION_IN_AMERICAN.2.aspx
15. Olin, J.W. and Sealove, B.A., 2010, July. Peripheral artery disease: current insight into the disease and its diagnosis and management. In Mayo Clinic Proceedings (Vol. 85, No. 7, pp. 678-692). Elsevier.
https://www.sciencedirect.com/science/article/pii/S0025619611601742
16. Reiman, M.P., Mather, R.C., Hash, T.W. and Cook, C.E., 2014. Examination of acetabular labral tear: a continued diagnostic challenge. British Journal of Sports Medicine, 48(4), pp.311-319.
https://bjsm.bmj.com/content/48/4/311.short
17. Tannast, M., Siebenrock, K.A. and Anderson, S.E., 2007. Femoroacetabular impingement: radiographic diagnosis-what the radiologist should know. AMERICAN JOURNAL OF ROENTGENOLOGY-NEW SERIES-, 188(6), p.1540.
https://www.researchgate.net/profile/Christopher-Straus/publication/11780817_Superselective_Microcoil_Embolization_of_Colonic_Hemorrhage/links/56956a6b08ae3ad8e33d6b09/Superselective-Microcoil-Embolization-of-Colonic-Hemorrhage.pdf
18. Woolf, C.J. and Mannion, R.J., 1999. Neuropathic pain: aetiology, symptoms, mechanisms, and management. The lancet, 353(9168), pp.1959-1964. https://www.sciencedirect.com/science/article/pii/S0140673699013070





