Arthritis is a broad-ranging term with numerous categories and classifications. Arthritis refers to the acute or chronic inflammation of a joint with pain and structural damage. Folks of all ages can be tormented by this condition.
If you are in knee pain without any history of trauma or accident, arthritis may be the factor generating the aching. In this article, we will be discussing some of the arthritis types giving rise to knee pain.
1. Osteoarthritis (OA)
Knee Osteoarthritis is commonly known as degenerative joint disease. It refers to the gradual erosion of the joint. People of older age are more prone to suffering from knee osteoarthritis. In general, females suffer from knee osteoarthritis more than males.

Knee OA is of two types.
Primary OA – unknown etiology. It can occur due to degenerative causes with aging.
Secondary OA – obesity, family history, genetic, previous untreated knee injury, joint hypermobility, prolonged immobilization, metabolic causes like rickets, structural problems like valgus or varus posture of the knee can influence the pathogenesis.
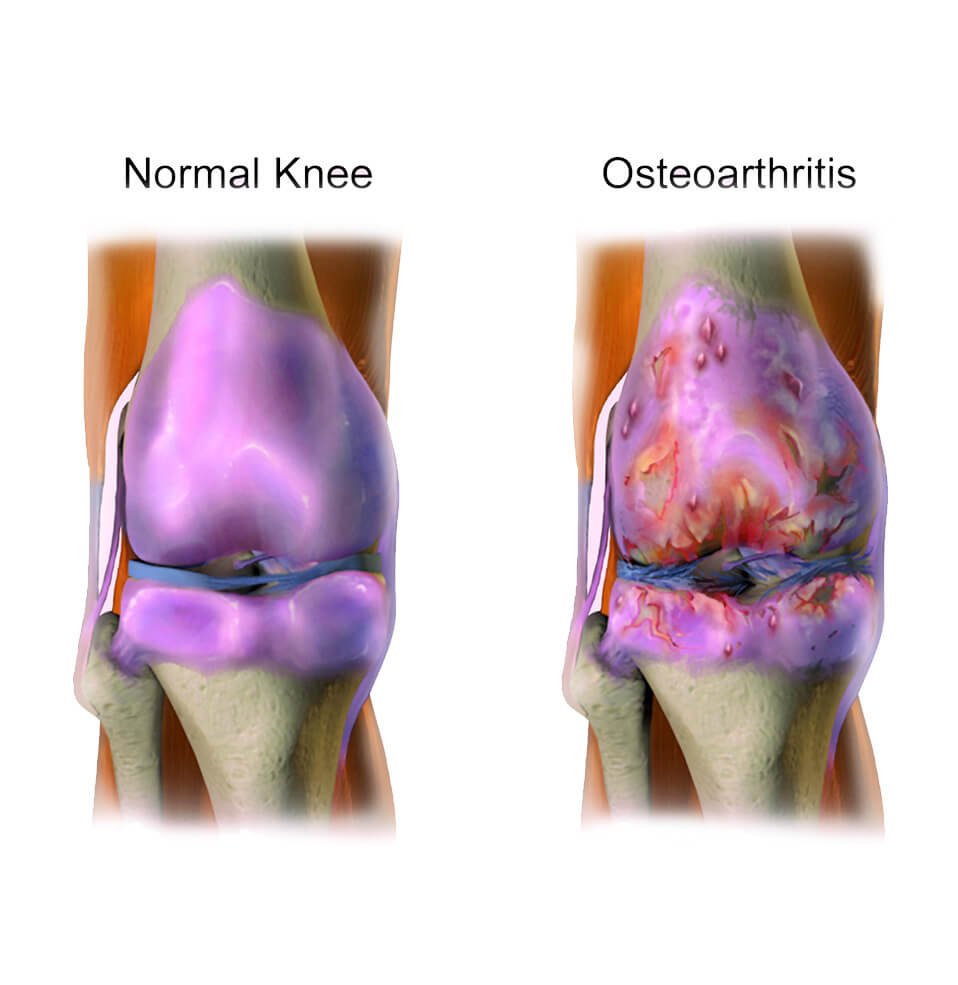
General signs and symptoms of knee OA are –
- pain during movement
- Joint stiffness, especially during the morning
- Pain while getting up after prolonged sitting
- Swelling around the knee joint
- Cracking sound while moving. It is termed ‘Crepitus’ in medical science.
- Pain during palpation
- In some cases, structural growth of the joint.
With the help of a blood test, X-ray, MRI, Knee osteoarthritis can be clinically diagnosed. The prime and evidence-based treatment protocol for knee osteoarthritis is physiotherapy. Physiotherapy treatment aims at:
- Lessen inflammation
- Minimize pain
- Strengthening muscle power around knee joint
- Sustain balance
- Lower the risk for cardiovascular diseases
To treat a knee OA patient, a physiotherapy doctor uses diverse therapeutic exercises, manual therapy, hydrotherapy, taping, massage, bracing, and electrotherapy. With proper physiotherapy intervention, it is possible to reduce further complications.
Read more: The Best Rehabilitation Exercises After Knee Surgery
2. Rheumatoid Arthritis
In rheumatoid arthritis, our body defense system works against us and attacks the joint tissues. Except for the genetic correlation, it is still unknown what may cause the disease. The female population is affected by the disease more than males.

The main sign symptoms for Knee Rheumatoid arthritis are:
- Pain in the knee joint
- Tenderness
- Feelings of discomfort while walking, running, doing exercises
Other symptoms are –
- Warm or temperature rise around the knee joint
- Joint stiffness especially in the winter or early in the morning after waking up from sleep
- Tingling sensation or numbness in the toe
Physical examination, Blood test, X-ray, MRI, Ultrasound are the diagnostic tools for confirming knee RA. Asides from other treatments, physiotherapy is beneficial for minimizing complications. The aims of physiotherapy treatment for a knee RA patient are:
- Educating the patient and his/her family about the disease
- Subdue pain
- Lessen joint stiffness as much as possible
- prevention of structural damage
- Increase muscle power
- Minimize general feeling of malaise, fatigue
- Enhance balance and coordination
To accomplish the above-mentioned goals, a physiotherapy doctor uses multifarious techniques like therapeutic exercise, TENS – Transcutaneous Electrical Nerve Stimulation, joint protection, hot/cold application, massage therapy, hydrotherapy, etc.
3. Psoriatic Arthritis
Psoriasis is a type of skin disease. Psoriatic arthritis is a chronic inflammatory joint disease that is allied with psoriasis. Both male and female populations can be affected by this condition. It can occur at any age. However, predominantly the 30-50 aged population is affected with psoriatic arthritis.
Researchers have found a combination of the genetic and environmental factors behind the occurrence of psoriatic arthritis. According to a 2017 review published in The New England Journal of Medicine – obesity, nail disease, traumatic event, smoking can influence the development of psoriatic arthritis.
People with psoriatic arthritis of the knee joint can face problems or complications like:
- Pain
- Stiffness
- Swelling
- Rise in temperature
Structures around the knee joint like bones, tendon, ligament, cartilage, skin, toes can also be affected. The patient might feel fatigued, have back pain, and have difficulties walking due to Achilles tendon pain.
Read more: Arthritis in knee

Physiotherapy plays a crucial role in improving the quality of life of a patient with this condition. Varying therapeutic exercise, cryotherapy, UV therapy, paraffin bath, hydrotherapy are in the physiotherapy management of psoriatic arthritis.
4. Gout and CPPD
Gout and pseudogout ( CPPD) are both metabolic disorders. But the signs and clinical manifestations of symptoms are closely matched with arthritis.
Both Gout and pseudogout occur due to different crystals. When there is an increased amount of Uric acid in the body, it results in the constitution of monosodium urate crystal resulting in pain. On the other side, CPPD stands for Calcium pyrophosphate dihydrate crystal deposition. In CPPD or pseudogout, crystals made of pyrophosphate dihydrate appear around the joint structure that causes pain.


Age, family history, a traumatic event can be the causative factors behind knee joint gout and pseudogout. Reportedly, the male population is affected with gout the most. People from 30-50 are the most affected age group. On the flip side, pseudogout can affect anyone over 60.
In both conditions, physiotherapy is an evidence-based treatment protocol. Asides from therapeutic exercise, splint, orthotics, cryotherapy, electroacupuncture techniques are used to treat both diseases.
5. Septic Arthritis
In this type of arthritis, due to bacterial infection,
- Joint pain
- Swelling
- Weakness
- fever – might be manifested.

In septic arthritis of the knee, asides from other interventions, Physiotherapy is an evidence-based treatment. Rehabilitation aims for this condition are as follows:
- Increasing muscular strength around knee joint
- Diminish pain
- Reduce joint stiffness
- Improving Joint Range Of Motion (ROM)
For this purpose, a physiotherapy doctor uses therapeutic exercise, joint mobilization, cryotherapy, hydrotherapy, joint splint, and pain management modalities according to the severity of the condition.
6. Reactive Arthritis
Formerly known as Reiter syndrome, this type of arthritis occurs after any gastrointestinal or genitourinary infection.
Symptoms like painful and swollen joints, sausage-like swelling of toes, fatigue might occur after several days or months of being infected. The older male population is affected by this arthritis the most.

If the knee joint is affected by this type of arthritis, physiotherapy can help with dealing with the complications.
FAQ’s
What are the main types of arthritis that affect the knee?
Osteoarthritis, Rheumatoid Arthritis, Psoriatic Arthritis, Gout and Pseudogout (CPPD), Septic Arthritis, Reactive Arthritis
What are the common symptoms of knee arthritis?
Pain during movement, Joint stiffness, Swelling around the knee joint, Limited range of motion, Crepitus (cracking sound while moving)
What are the risk factors for developing knee arthritis?
Age, Gender, Obesity, Family history, Previous knee injury or trauma, Genetic predisposition
How is knee arthritis diagnosed?
Diagnosis is typically made through a combination of physical examination, patient history, blood tests, X-rays, and other imaging techniques such as MRI or ultrasound.
What are the main treatment options for knee arthritis?
Medication for pain relief and inflammation, Physical therapy and exercise, Assistive devices, such as braces or orthotics, Weight loss, if necessary in some cases, joint injections or surgery
Can knee arthritis be prevented?
While some risk factors, such as age and genetics, cannot be controlled, maintaining a healthy weight, staying active, and avoiding joint injuries can help reduce the risk of developing knee arthritis.
Can knee arthritis be cured?
There is currently no cure for arthritis, but with proper management and treatment, many people can effectively manage their symptoms and maintain a good quality of life.
What is the role of physiotherapy in managing knee arthritis?
Physiotherapy aims to reduce pain, improve joint mobility, increase muscle strength, and enhance balance and coordination through various techniques such as therapeutic exercises, manual therapy, hydrotherapy, and electrotherapy.
When should I consult a doctor for knee pain?
If you experience persistent or worsening knee pain, swelling, stiffness, or reduced range of motion that is not relieved by rest or over-the-counter pain medication, it is advisable to consult a healthcare professional for further evaluation and treatment.
Can knee arthritis lead to knee replacement surgery?
In severe cases of knee arthritis, where conservative treatments have not provided sufficient relief, knee replacement surgery may be considered to improve function and alleviate pain.
Sources
- Bijlsma, J.W., Berenbaum, F. and Lafeber, F.P., 2011. Osteoarthritis: an update with relevance for clinical practice. The Lancet, 377(9783), pp.2115-2126. https://www.sciencedirect.com/science/article/pii/S0140673611602432
- Ritchlin, C.T., Colbert, R.A. and Gladman, D.D., 2017. Psoriatic arthritis. New England Journal of Medicine, 376(10), pp.957-970. https://www.nejm.org/doi/full/10.1056/nejmra1505557
- Kuo, C.F., Grainge, M.J., Zhang, W. and Doherty, M., 2015. Global epidemiology of gout: prevalence, incidence and risk factors. Nature reviews rheumatology, 11(11), pp.649-662. https://www.nature.com/articles/nrrheum.2015.91
- Rosenthal, A.K. and Ryan, L.M., 2016. Calcium pyrophosphate deposition disease. New England Journal of Medicine, 374(26), pp.2575-2584. https://www.nejm.org/doi/full/10.1056/NEJMra1511117
- Horowitz, D.L., Katzap, E., Horowitz, S. and Barilla-LaBarca, M.L., 2011. Approach to septic arthritis. American family physician, 84(6), pp.653-660. https://www.aafp.org/afp/2011/0915/p653.html?utm_medium=email&utm_source=transaction
- Carter, J.D. and Hudson, A.P., 2009. Reactive arthritis: clinical aspects and medical management. Rheumatic Disease Clinics, 35(1), pp.21-44. https://www.rheumatic.theclinics.com/article/S0889-857X(09)00011-8/abstract
- Shirtliff, M.E. and Mader, J.T., 2002. Acute septic arthritis. Clinical microbiology reviews, 15(4), pp.527-544. https://journals.asm.org/doi/abs/10.1128/CMR.15.4.527-544.2002





